CHAPTER I
INTRODUCTION
Testicular abnormalities are quite often one of them is this testicle torsion. Thus the need for a more detailed discussion.
In anatomy, testis is the male genital organ teletak in the scrotum. Tetstis size in adults is 4 x 3 x 2.5 cm. with ovoid-shaped volume of 15-25 ml. Both pieces of testicular tissue enveloped by the tunica albuginea are attached to the testis. Outside there albugine tunica vaginalis tunica composed of visceral and parietal layers, and the tunica dartos. Kremaster muscles that surround the testes allow the testes to the abdominal cavity can be driven approach for maintaining testicular temperature to remain stable.
In histopathologic, testis lobuli consist of ± 250, and each lobule consists of seminiferi tubule. In the seminiferous tubules contained spermatogonia cells and Sertoli cells, being in between there seminiferi tubule Leydig cells. Spermatogonial cells in the process of spermatogenesis to sperm cells. Sertoli cells would serve to feed the sperm, whereas the Leydig cells called interstitial cells of testis function in producing hormone testosterone.
Sperm cells are produced in the testis tubule seminiferi stored and maturation / maturation in the epididymis. Once mature (adult) sperm cells together with the sap of the epididymis and vas deferens is channeled toward the ampulla vas deferens. The cells after mixing with fluids from the epididymis, vas deferens and seminal vesicles, and prostate fluid, semen or seminal fluid form.
Testicular blood received from several branches of the artery, internal spermatic artery is a branch of the aorta, the artery deferensialis branch of the inferior vesical artery, and arteries that branch kremasterika epigastric artery. The left testicular vein left testis converge to form assembled pampiniform plexus. Plexus is dilated in some people and is known as varicocele. (2)
CHAPTER II
DISCUSSION
I. DEFINITION
Testicular torsion is terpeluntirnya funikulus spermatikus which cause the interruption of blood flow to the testis. This situation affects the I among 4000 men aged less than 25 years, most common in children during puberty (12-20 years). Besides that, not infrequently the fetus is still in the uterus or the newborn suffering from undiagnosed testicular torsion resulting in loss of both unilateral and bilateral testes. (2)
Testicular torsion or terpeluntirnya funikulus spermatikus which can cause strangulation of the blood vessels, occurs in the tissue surrounding the male testes do not adhere well to the scrotum.Testicular atrophy may infarction and experience if it does not get the blood flow more than six hours.(5)
II. Etiology
Testicular torsion occurs when a testicle can move very freely. Free movement is found in the following circumstances:
1. Mesorchium long.
2. Testis tendency to be in a horizontal position.
3. The epididymis is located at one pole of the testis. (3)
In addition to a very free motion, excessive movement of the testicles can also cause testicular torsion. Some circumstances may cause excessive movement, among others; sudden temperature changes (such as swimming), fear, excessive exercise, coughing, pants are too tight, defecation or trauma of the scrotum.
On the fetus and neonate, which attaches to the muscular layer of dartos tissue is still not a lot of buffer so that the testis, epididymis and tunica vaginalis is easy to move and allow for on-axis terpeluntir funikulus spermatikus. Terpeluntirnya testis in a condition called testicular torsionekstravaginal . (2)
The occurrence of testicular torsion in adolescence is associated with many disorders testis buffer system. The tunica vaginalis testis should be around most of the anterior and lateral surface of the testis, in these circumstances surround the entire surface of the tunica testis thus preventing the insertion of the epididymis to the scrotum wall. This condition causes the testis and epididymis easily move in and hang the bag on the tunica vaginalis funikulus spermatikus. This condition is known as anomalous bell Clapper . This condition causes the testis prone to torsion intravaginal . (2)
Patients with testicular torsion may experience the following symptoms:
1. Sudden severe pain in one testicle, with or without predisposing factors
2. Scrotum is swollen on one side
3. Nausea or vomiting
4. Mild headache (7)
At the beginning of the process, has not been found swelling of the scrotum. Testicular infarction may lead to changes in the scrotum. Scrotum will be very painful redness and swelling. Patients often have difficulty finding a comfortable position. (6)
Besides pain in the side of the testicular torsion experienced, can also be found referred pain in the groin or abdominal area. If testicular torsion is experiencing undesendensus testis, the symptoms that arise resembles Strangulated hernia. (3)
IV. PHYSICAL EXAMINATION
In phisical examination, which had torsion testis is located higher and more horizontal than the contralateral side of the testis. Sometimes the new testicular torsion occurs, the coil can be touched or thickening funikulus spermatikus. This situation is usually not accompanied by fever. (2)
Right and left testis testis should be equal. Asymmetric enlargement, especially if it occurs acutely, indicating the possibility of a pathological condition in one testicle. Scrotum skin discoloration, can indicate a problem. The last thing to watch out for is any pain or discomfort in the testicles. (6) Reflex cremaster is generally lost in testicular torsion. The absence of reflex kremaster, 100% sensitive and 66% specific in testicular torsion. In some boys, kremaster reflex may decrease or no from the beginning, and kremaster reflex can still be found in cases of testicular torsion, therefore, the presence or absence of reflex kremaster can not be used as the sole reference to diagnose or rule out a diagnosis of testicular torsion. (5)
V. Examination support
Investigations are useful to differentiate testicular torsion acute scrotum with the other is to use a Doppler stethoscope, Doppler ultrasonography, and sintigrafi testis, all of which aim to assess blood flow to the testicles. (2) Unfortunately, Doppler stethoscope and conventional ultrasonography is not very useful in assessing the blood flow to the testicles. Testicular blood flow assessment in nuclear can help, but it takes a long time so the case can be delayed. Color Doppler ultrasonography is a noninvasive examination of the accuracy is approximately proportional to the examination of nuclear scanning. Color Doppler ultrasound to assess blood flow, and can distinguish blood flow and blood flow intratestikular scrotum wall. This tool can also be used to check for other pathological conditions of the scrotum. (8)
Color Doppler ultrasonogram showing acute torsion affecting the left testicle in a 14-year-old boy had acute pain WHO for four hours. Note Decreased blood flow in the left testis compared with the right tstis.

 Color Doppler ultrasonogram showing late torsion affecting the right testis in a 16-year-old boy WHO had pain for 24 hours. Note Increased blood flow around the right testis but absence of flow within the substance of the testis
Color Doppler ultrasonogram showing late torsion affecting the right testis in a 16-year-old boy WHO had pain for 24 hours. Note Increased blood flow around the right testis but absence of flow within the substance of the testisColor Doppler ultrasonogram showing inflammation (epididymitis) in a 16-year-old boy in the WHO had left testicular pain for 24 hours. Note Increased blood flow in and around the left testis
Examination of urine sediments showed no leukocytes in the urine, and blood examination showed no inflammation except in torsion long and had sterile inflammation. (2)
VI. DIAGNOSIS (8.9)
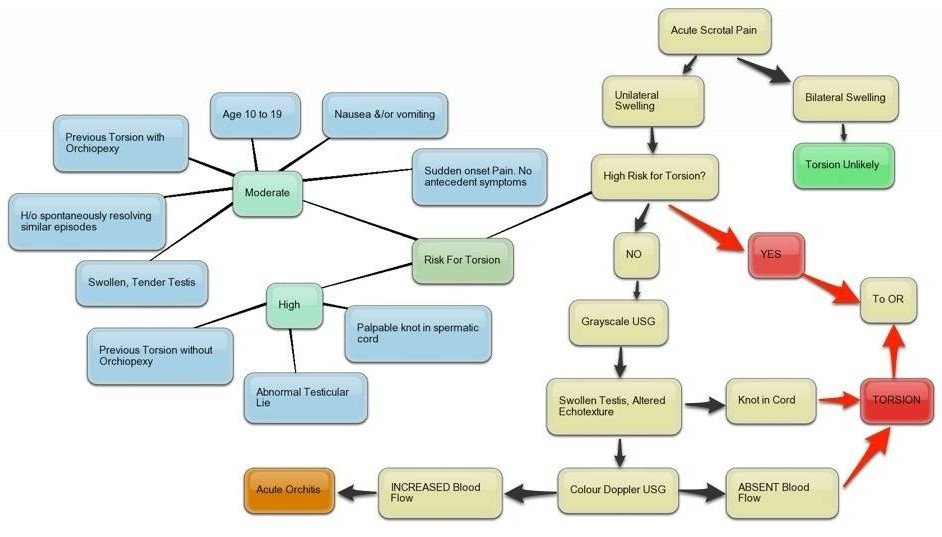
Diagnosis begins with a history of testicular torsion, physical examination, and investigations. In general, the algorithm described in the chart and Testicular Torsion Clinical Pathway as follows:
VII. DIAGNOSIS (1,2,4,5)
1. Acute epididymitis. The disease is generally difficult to distinguish from testicular torsion.Acute scrotum pain usually accompanied by a rise in temperature, a discharge of pus from the urethra, a history of coitus suspectus (other than the alleged intercourse with his wife), or had undergone previous urethral catheterization. On examination, epididymitis and testicular torsion, can be distinguished by Prehn's sign, ie if the testes are exposed to elevated, at epididmis sometimes acute pain will be reduced (Prehn's sign positive), while the torsion of testicular pain persists (Prehn's sign is negative). Patients Acute epididymitis is usually more than 20 years old and on examination of urine sediment obtained leukosituria and bacteriuria.
2. Incarserata scrotalis hernia. In the anamnesis obtained a history of lumps that can come out into the scrotum.

5. Edema of the scrotum that can be caused by hipoproteinemia, filariasis, inguinal lymph channel obstruction, cardiac abnormalities, or abnormalities of unexplained (idiopathic).
The difference between testicular torsion, torsion appendix testis and epididymitis can be seen in the table below. (8)
Diagnosis of Selected Conditions Responsible for the acute scrotum
Condition | Onset of symptoms | Age | Tenderness | Urinalysis | Cremasteric reflex | Treatment |
Testicular torsion | Acute | Early Puberty | Diffuse | - | + | Surgical exploration |
Appendiceal torsion | Subacute | Prepubertal | Localized to upper pole | - | + | Bed rest and scrotal elevation |
Epididymitis | Insidious | Adolescence | Epididymal | + / - | + | Antibiotic |
VIII. MANAGEMENT / management
A. Non-operative
In some cases of testicular torsion, detorsi manual of funikulus spermatikus can restore blood flow.(5)
Detorsi manual is to return to the original position of the testis, with testis detour in the opposite direction to the direction of torsion. Because the direction of torsion is usually the medial, it is recommended to rotate the testis to the lateral direction first, then if nothing changes, try detorsi medial direction.
The method is known as the "open book" (to the right testis), because movements like opening a book. If successful, the pain may disappear in most patients. Detorsi manual is the best way to prolong the time waiting for surgery, but can not avoid the surgical procedure. (2.5)
In practice, manual detorsi difficult and rarely done. In the emergency room, the child with a swollen and painful scrotum, the action is hard to do without anesthesia. In addition, the testis may not be fully terdetorsi or torsion can return to shortly after the patient goes home from the hospital. In addition, knowing the direction in which the testes have torsion is almost impossible, which led to the manual detorsi action would worsen the degree of torsion. (5)
2. Operative
Testicular torsion is an emergency case, every effort should be made to accelerate the process of surgery. The results of surgery depend on the duration of ischemia, therefore, time is critical. Usually time wasted on imaging studies, laboratory, or other diagnostic procedures that resulted in the testis can not be maintained.
The purpose of exploration are:
1. To confirm the diagnosis of testicular torsion
2. Do detorsi testicular torsion
3. Check whether the testis is still viable
4. Throw (if the testis was nonviable) or fixate if the testes are still viable
5. Fixate the contralateral testis
Differences on measures of exploration is partly due to the low likelihood of testicular torsion is still viable if long-standing (> 24-48 hours). Some experts still maintain the opinion to continue to explore the grounds medikolegal, the exploration is needed to prove the diagnosis, to save the testicle (if still possible), and to perform orchidopexy on the contralateral testis. (5)
When the surgery, performed also preventive measures on the contralateral testis. This is done because testicular torsion kontralaeral have a chance next time. (3,5,7)
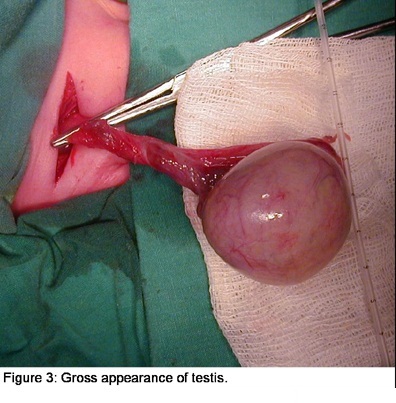
If the testis is still viable, do orchidopexy (testicle fixation) in the tunica dartos was followed on the contralateral testis. Orchidopexy is done by using a thread that is not absorbed in the three places to prevent the testes do not twist again. Whereas in testis which had suffered necrosis, performed removal of the testicles (orchidectomy) and then followed the contralateral orchidopexy. Who have undergone testicular necrosis if it remains in the scrotum can stimulate the formation of antibodies antisperma thereby reducing the ability of fertility later in life. (2)
IX. COMPLICATIONS (5)
1. Atrophy of the testis
2. Recurrent torsion
3. Wound infection
4. Subfertility
REFERENCES
(1) Blandy, John. Lecture Notes on Urology. Third edition. Oxford: Blackwell Publication Scietific. Of 1982. 277.
(2) Purnomo, Basuki P. The basics of Urology. New York: Sagung Seto. , 2003. 8.145 to 148.
(3) Scott, Roy, Deane, R.Fletcher. Ilustrated Urology. London and New York: Churchill Livingstone. In 1975. 324-325.
(4) Sjamsuhidajat R, Wim De Jong. Textbook of Surgery . Second edition. New York: Medical Books - EGC. , 2004. 799.





















It was my last hope of having a child and Dr Obodo made my dreams come true. I asked for the spells, but didn’t tell my husband. We carried on trying to get pregnant as normal. I had a really good feeling about Obodo. I felt pregnant or like pregnancy was coming very about a week after the spells were cast. I began to vomit in the morning from morning sickness. I thought it was the toast. I’ve never felt like that before. And it was true! I went and grabbed the pee stick to show my husband. I went to my doctors at the earliest possible time to have a test and it came back positive. I immediately rang up my husband to let him know that the pee stick was not a false positive. He asked me how it was possible. He was certain that the pee stick was passed the expiry date. I told him all about Obodo, the fertility spells and he was amazed. We now have a very beautiful baby boy on the way and we are expecting to use Obodo in hope that I can have my baby girl. you can get in touch with doc via info ___ templeofanswer@hotmail . co . uk , call 234 8155 425481 for help
ReplyDeleteThank you,
The Messer Family
The reasons comprise infective contagion, viral infection and, less typically, chemical irritation. Treatment normally includes antibiotics, painkillers and anti-inflammatory treatment. Full retrieval can take place in just a few days. Early Analysis of Epididymitis means early Epididymitis cure. Make sure you get a remedial diagnosis and Natural Remedies for Epididymitis.
ReplyDelete