HYPOSPADIA
I. INTRODUCTION
I.1. Embryology
At the age of 2 weeks a new embryo contained two layers of the ectoderm and entoderm. Only then formed indentation in the middle - the middle of the mesoderm which then migrate to the periphery, separating the ectoderm and entoderm. In the caudal ectoderm and entoderm remain united to form cloacal membrane. At the beginning of week 6, the protrusions are formed between the umbilical cord and the tail is called the genital tubercle. Formed underneath the indentation where the center line of the lateral section there are two elongated folds called the genital fold. During week 7, the genital tubercle will elongate and form the glans. It is the primordial form of the penis when the embryo is male. When the woman would be the clitoris.
If there is agenesis of the mesoderm, the genital tubercle was formed, so that the penis is also not formed. Bagisan anterior of the cloacal membrane, the membrane will rupture and form urogenitalia sinus. Meanwhile, a pair of folds called the genital fold will form the sides of the sinus urogenitalia. When the genital fold failed to unite over the sinus will arise urogenitalia hypospadias. During this period, formed genital swelling in the lateral left and right. Hypospadias is the hardest type of penoskrotal skrotal and perineal, occurs due to failure to fold and genital sweling to unite in the middle.
Figure 1. anatomy of the penis
Normal anatomy of the penis consists of a pair of the corpora cavernous tunica covered by a thick and fibrous albugenia with a septum in the middle. Urethra through the penis in the corpus spongiosum which lies in a ventral position in the groove between the corpora cavernous. Urethra appears at the distal end of the conical shaped glans penis. Spermatic fascia or tunica dartos, is a loose layer of the penis, located on the fascia. Under the tunica dartos Bucks are facia that surrounds the corpora cavernous and then split to cover the corpus spongiosum separately. Dorsal neurovascular beam lies in the Bucks fascia between the two corpora cavernous.
I.3.Definition
Hypospadias comes from the Greek, Hypo meaning under, Spadon which means the gap. Hypospadias is a congenital abnormality in which the external urethral meatus is located on the ventral surface of the penis and more proximal than the normal place (tip of the penis gland). Estuary of the urethra may also be located in the scrotum or perineum. The more proximal to the penile urethra defect will be more experienced shortening and curvature form of so-called "chordee". Hypospadias deficiency leads to various levels of the urethra. Fibrotic tissue that cause chordee replace fascia and tunica dartos Bucks. Skin and prepuce on the ventral part becomes thin, imperfect and form a dorsal hood over the glans (Duckett, 1986, Mc Aninch, 1992). Hypospadia in the community so that children like to be called circumcised from birth by a ghost. The incidence of hypospadias is 1: 350 births male - male. With distal hypospadias percentage: 80-90% and proximal hypospadias 10-20%.
I.4. Etiology
One of the congenital abnormalities of the penis is the second most after undescensus testiculorum (cryptorchidism) is hypospadias. The incidence of hypospadias is influenced by many factors including genetic, hormonal, racial, geographic, and now that should receive special attention, namely the influence of environmental factors that pencemran industrial waste.
Aetiology is not known for sure, alleged failure of the testes to produce testosterone in sufficient numbers play a role in hypospadias. Similarly, the presence of the cell - the cell structure of genital deficiency of androgen receptors are also cells - cells lack the enzyme 5 alpha reduktesesehingga androgen stimulation to change testosterone to dihydrotestosterone be inadequate to trigger the onset of one of hypospadias. According to the 2000 Silver genetics, endocrinology and environment are factors that play a role in the incidence of hypospadias.
Some of the possibilities is associated with hypospadias, namely:
• Failure bud ectoderm cells derived from the tip of the glans to grow into the mass of the glans joins the
entoderm cells along the penile urethra. This resulted in the urethra eksternum osteum located in the glans or
corona glandis on the ventral surface.
• Failure to cover the genital folds merging flow urethra - urethral groove into the penile urethra resulting in
urethral osteum eksternum located in the shaft of the penis. Similarly, the failure of the genital tube together
with a perfect result osteum empties into the urethra ekternum penoskrotal or perineal.
I.5. Pathogenesis
Hypospadias occurs as a developmental disorder of the anterior urethra is not perfect so that the urethra is located anywhere along the shaft of the penis to the perineum. The more proximal the mouth of the meatus, the greater the possibility of ventral penile shortening and curved because of the chordae.
Until recently the occurrence of hypospadias is still considered to be due to androgen deficiency or excess of estrogen in masculinization of the embryonic process Devine, 1970 said that the deformities that occur in patients with hypospadias is caused by involution interstitial cells of the testis that is growing, along with the cessation of androgen production, resulting in maskulanisasi imperfect organs of the external genetalia There are many factors that cause hypospadias and a lot of the theory about the cause of hypospadias among others:
• Genetic factors
12% effect on the incidence of hypospadias when the family have had a history of hypospadias. 50% effect
on the incidence of hypospadias when his father suffered from hypospadias.
• ethnic and geographic factors
In the United States the incidence of hypospadias in the Caucasian higher than the African Americans are
1.3
• Hormonal factors
Factor of androgen / estrogen affects the incidence of hypospadias because it affects the process of
masculinization of the embryo. Sharpe and Kebaek (1993) put forward a hypothesis about the effect of
estrogen on the incidence of hypospadias that estrogen plays an important role in the formation of male
external genital embryonal moment.
Changes in estrogen levels can be derived from:
• Androgens are dietary changes that increase the body is weak.
• Synthetics such as oral kontracepsi (Ethynil Estradiol)
• Plants such as soybeans
• Estrogen like compounds chemical organochlcrin
Androgens produced by the testes and the placenta due to androgen deficiency will cause a decrease in production dehidrotestosterone (DHT) which is influenced by 5 α reductase, was instrumental in the formation of the penis so that when androgen deficiency will lead to failure of formation of the urethra tube called hypospadias.
• Factors industrial waste pollution
Industrial waste acted as "Endocrin discrupting chemicals" are good as well as anti-androgenic eksogenik like polychlorobiphenyls, dioxins, furans, peptisida organochlorin, alkilphenol polyethoxsylates and phtalites.
It is known that the level of indifference after the development of external male genital further influenced by the estrogen produced by the testes primitive. One hypothesis suggests that estrogen deficiency or the presence of anti-androgen will affect the formation of male genitalia ekterna.
II. classification
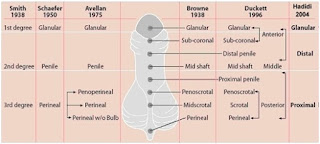
Classification of hypospadias is often used is based on the location of the meatus is:
1. Glandular, estuary located on the proximal penis penis glands
2. Coronal, located at the mouth of the penis sulcus coronalia
3. penile shaft
4. Penoscrotal
5. Perineal.
Based on the location of the mouth of the urethra after chordee correction, Brownee (1836) hypospadias divided into three major parts, namely:
1. Anterior hypospadias, which consists of glandular type, subchondral, and the distal penis.
2. Medius consists of midshaft hypospadias, and the proximal penis.
3. Consists of posterior hypospadias penoskrotal, scrotal, and perineal.
Paulozzi et al, 1997 where the Metropolitan Congenital Defects Program (MCDP) divides the 3-degree hypospadias, namely:
• The degree I: Oue lies on the ventral surface of the glans penis and corona glandis.
• Grade II: Oue is located on the ventral surface of the shaft of the penis
• Grade III: Oue is located on the ventral surface of the scrotum or perineum
Usually the degree II and degree III followed by curling into the ventral penis called chordee. Chordee is due to too short, the skin on the ventral surface of the penis. These degrees of hypospadias will disrupt the normal flow of urine and reproductive function, therefore it needs to be done with surgical therapy.
Diagnosis
Anamnesis
In adults who suffer from hypospadias may complain of difficulty directing jets of urine. Chordee can cause the curve to the ventral shaft of the penis that can interfere with sexual intercourse. Perineal and penoscrotal type hypospadias cause micturition the patient must be in a sitting position, and this type of hypospadias can lead to infertility.
The clinical manifestations
In most patients there is a penis is curved towards the bottom that will appear more clearly at the time of erection. This is caused by the presence of chordee, which is a fibrous tissue that spreads from the start to the meatus is abnormally located gland penis. This fibrous tissue is a rudimentary form of the urethra, the corpus spongiosum and the tunica Dartos. Even though the presence of chordee is one hallmark to suspect a hypospadias, keep in mind that not all have hypospadias chordee.
Investigations
Diagnosis of hypospadias is usually apparent on examination of the inspection. Sometimes hypospadias can be diagnosed on prenatal ultrasound examination. If not identified before birth, it usually can be identified on examination after birth.
Some investigation to do is urethtroscopy and cystoscopy to ensure the internal sex organs are formed normally. Uretroskopi and cystoscopy also assist in evaluating the development of the internal reproductive organs. Excretory urography performed to detect the presence or absence of congenital abnormalities of the kidney and ureter.
III. Management
The management of hypospadias is by surgery. Purpose of the procedure in hypospadias surgery are:
1. Make a straight penis with fixing chordae
2. Form the urethra and meatusnya that lead to the tip of the penis (Uretroplasti)
3. To restore the normal aspects of the external genitalia (cosmetic)
two main things in hypospadias repair, namely:
Chordectomi, released chordae can be straight forward so that the penis when erect.
Urethroplasty, making osteum externa urethra tip of the penis gland so that urine and semen emission can be straight forward.
If chordectomi and urethroplasty performed in one operation the same time is called a stage, when done in a different time called the two-stage
There are four things to consider in planning for hypospadias repair surgery can be achieved for the purpose of the age, type of hypospadias and penis size and the presence or absence of chorde. Ideal age for hypospadias repair is age 6 months to school age not because of psychological factors to consider surgery and the child's disorder itself, so the stage hypospadias repair was accomplished before the child's school.
Surgery is performed under circumstances malformasinya. Glanular hypospadias distal urethra on there that are not formed, usually without recurvatum, this form can be reconstructed with local flap (eg, procedures Santanelli, Flip flap, MAGPI [meatal advance and glanuloplasty], including the prepuce plasty).
There are three types of reconstruction as follows: The type of hypospadias and penis are very influential on the stages and techniques of this operation affects the success of the operation. The smaller the penis and getting into the more proximal hypospadias type of technical difficulty and the success of its operations.
o Methods Duplay
To type penil hypospadias repair.
Skin penil used to make urethrop lastinya or scrotum skin can also be used.
o Methods Ombredane, for coronal and distal hypospadias repair penil.
o Nove-josserand, for various types of hypospadias repair using a skin graft but urethroplastinya.
Purpose of hypospadias repair to release the chordee and put back native urethra or the urethra to form the
tip of the glans penis. One of the most important problems in hypospadias surgery is the difficulty in forming
a new urethra meatus. Skin designed by graff first uretroplasty Nove - Joserand. However, because of
potential complications such as stenosis, so at this time is not used anymore.
Duplay Thiersche and perform a two-stage repair in which the first stage of cutting layers that cause chordee and straighten the penis. A few months later the urethra is formed by cutting lengthwise down the ventral surface of the penis to form a urethra. The weakness of this operation that the technique does not extend to the tip of the glans urethra.
Cecil introduced the technique of hypospadias repair in which the three stages in the second stage of the penis is attached to the scrotum. Only in the third stage to separate the penis and scrotum
In all these techniques in the first phase of the operation is performed excision of the chordee. Wound closure operation is performed by using prepuce skin of the dorsum of the penis. The first stage was conducted at the age of 1.5 - 2 years when the penis size according to age. After excision of the chordee penis will be straight, but the meatus is positioned as abnormal. In the second stage of the work done uretroplasty 6 months after the first stage.
The most popular repair techniques performed by a plastic surgeon is a surgery modification techniques Thiersch - Duplay. Excess tissue is transferred from the dorsum of the penis prepuce to the ventral surface. Byar, 1951 to modify this operation by splitting the prepuce on the center line and bring it to the prepuce flap distal ventral surface of the penis. It thus provides the advantages of networking to further rekontroksi urethra. After intervals of at least 6 months, a central strip of skin attached to the ventral surface of the penis, and tube strip of skin is pulled as far as possible toward the distal. Byar can cover the new urethra with lateral skin edges together in the midline with the closing of the coated layer.
Engineering Thirsh - duplay modified by byar
1. Is a penis with chordee.
2. Incision in the linea media from urethral meatus to the corona and around the glans penis from the proximal
side.
3. Cut tissue causing chordee. Incision was made in such a way that it lies in linea from proputium media that
is not folded.
4. The skin flap is transferred to the ventral prepuce.
5. At the second stage, a central strip is isolated to form the urethra. Network behind the flap is loose enough
for the formation of tube.
6. Tubules (tube) has been formed, a circumcision is performed and the incision of the lateral skin flap is used.
7. But from the flap diperdekatkan with different cover.
8. Then brought near the skin edges.
.
The second stage surgery, Browne 1953 an incision parallel to the ventral surface of the penis that extends from the meatus penis Valentine. This will isolate the strip incision in the skin of the midline. Width depending on the desired caliber of the new urethra. Skin lateral to the midline diperdekatkan further to cover the strip of skin is immersed. Relaksing incision lateral dorsal skin will allow it to each other without causing tension , however this technique has the possibility of the occurrence of fistula and stenosis that followed only for the experienced surgeon
Culp, 1959 to modify the way the surgery was performed by Cecil, 1955. In the first stage of operation is released after recovery chordee, the urethra is formed by making the central vessels of the skin on the ventral surface of the penis, as Thiersch technique - Duplay and cover the rough surface of the penis by way of instilling it in the bag is made in sokrotum. End of the penile skin and subcutaneous tissue above the urethra into the layers together diperdekatkan skrotal. With a few stitches. Anastomosis-penil Skorotal then separated, leaving a lot of skin on the penis skrotal to cover the ventral surface.
Repair actions performed before the child is school age. 1.5 to 2 years. Before uretroplasty all tissues that cause chordee should be discarded. After that testing be done if the chordee artifical erection persists despite these efforts have been made, further resection is performed on urine diversion layer for distal Hypospadias repair is done by the small size Foley catheter no. 8. For 3 to 4 days. Penile hypospadias, whereas the preferred periental uretrostomy skrotal and perineal Hypospadias can didiversi with suprapubic drainage.
Distal Hypospadias Techniques section
Hypospadias repair is performed if the type of v-flap of the glans tissue reached normal urethra after chordee correction, urethral made of 'Flip - Flop "skin. This flap will form the ventral and lateral sides of the urethra and the sewing on the v-shaped flap of tissue on the glans, which will complete the top and the sides of the new urethra. Several sutures are placed behind the v-flap attached to the granular surface of the dorsal urethral incision to open the original meatus. Lateral wings of the glans tissue is under the direction and brought near the ventral midline. Ventral surface of the lid with a penis in the prepuce. The tip of the flap is usually excessive and should be cut. Here you should use a flap to form a surface on the back of the center line.
Granular Z-shaped flap design can also be done to obtain the meatus which both cosmetic and functional form of 2 was held on the cutting tip of the glans in the center position upwards. The ratio of the Z dimension to the dimensions of the glans is 1: 3, Two flap is placed horizontally on opposite sides. After releasing the chordee, a two-sided flap is used to form the new urethra and to close the ventral surface of the penis, the inner surface of the prepuce is prepared for the extension of the urethra. To mentransposisikan new urethra, the channel is formed above tinika albuginia to the glans. The external urethral meatus to the glans carried through these channels. Distal part of the urethra is cut on the anterior and posterior to the vertical direction of the flap Trianggular incorporated into the fissure and stitched with thread 6-0 poly glatin. After the flap is then inserted and sutured to the glans urethra anastomosis could be completed.
Proximal Hypospadias Techniques section
When the flap can not reach the urethra granular exist, then a graph can be used to extend the porters urethra. Furthermore normal urethra calibrated to determine its size (usually 12 French children aged 2 years). The corresponding segment of skin taken from the distal tip of the prepuce. Graft is then sutured to the rough surface facing out, on a catheter or tube pipe is made that at the end of proksimalnya must comply with a long slit meatus urethra with sutures and the flap granular unbroken thread kromic gut 6-0, lateral wing of the then mobilized toward granular tissue distal urethra to close the channel and back over the glans to form a new urethra will meet at the tip of the glans.
Complication
Complications arising post hypospadias repair is influenced by many factors including patient age, type of hypospadias, the stages of operation, precision engineering operation, and maintenance of post-hypospadias repair. Kinds of complications that occur are:
• Bleeding
• Infection
• fistula urethrokutan
• Stricture urethra, urethra stenosis
• diverticular urethra.
The most frequent complication of repair hipospodia is fistula, diverticulum, urethral stricture and meatal stenosis (Ombresanne, 1913). The most common cause of fistula is necrosis of the flap caused by the accumulation of blood under the flap. Fistula can be allowed to heal spontaneously with secondary repair 6 months later. To be on the verge of defeat that should be worn for 2 weeks after fistulanya recovered, with the hope of the edges will reunite, while the continued diversion of its usefulness for longer than two weeks.
Narrowing of the urethra is a problem. If the narrowing is solid, then the dilatation of the urethra will be effective. In the great narrowing, secondary surgery is required. Internal Urethrotomy be adequate for a short constriction. Medium to long narrowing of the urethra should be opened along the constriction region and the full thickness of skin graft used to reconstruct the size of the urethra can be on the verge of defeat A are used to support a skin graft.
Prognosis
Anesthesia, sewing equipment, antibiotics support the success of hypospadias surgery. After surgery, urination can be done with a straight penis and deposit semen into the vagina. The biggest challenge is the correction of hypospadias fistula prevention and overall cosmetic picture.
REFERENCES
1. Sjamsuhidajat R, De Jong Wim. Buku Ajar Bedah. Ed2. Jakarta : Penerbit Buku EGC.2004.Hal 747
2. Sabiston D, Oswari J.Buku Ajar Bedah. Jakarta : Penerbit EGC.1994.Hal 488
3. Doherty GM. Current Surgical Diagnosis and Treatment. USA : McGraw Hill.2006.Page 1007-1008
4. Schwartz. Intisari Prinsip-prinsip Ilmu Bedah. Jakarta : EGC 2000. Hal 590
5. Purnomo, S,Basuki. Dasar Dasar Urologi Edisi 2 .Jakarta : CV. Sagung Seto.2009. Halaman 152-153.
6. Anonim. Hipospadia. Diunduh tanggal 17 April 2010. Tersedia di URL: .bedahugm.net/hipospadia
7. Anonim. Hipospadia. Diunduh tanggal 17 April 2010. Tersedia di URL:.oktavianus.multiply.com
8. Prihantono.Hipospadia. Diunduh tanggal 17 April 2010. Tersedia di URL: cribd.com/doc/16606301/




ReplyDeleteGod bless Dr.OLU for his marvelous work in my life, I was suffering for hypospadias since child hood and I was taking my medications and i wasn't satisfied and about to go for suddery, i needed to get the hypospadias out of my body, I searched about some possible cure for hypospadias and i saw a comment about Dr. OLU, how he cured a man with his herbal medicine, I contacted him and he guided me. I asked for solutions, he started the remedy for my health, he sent me the medicine through UPS SPEED POST. I took the medicine as prescribed by him and 7days later it was cleared, Dr. OLU truly you are great, do you need his help also? Why don't you contact him through drolusolutionhome@gmail.com
call or what-apps him through +2348140654426. .he also specialize on the following things
hirschsprungs disease
Hepatic B
Cancer
Penis growth
Thanks for the cure sir, you indeed save my life...I am really grateful sir,